The genocide in Gaza is ‘another level of annihilation’
In this Q&A with Prism, Dr. Mimi Syed discusses her two missions to Gaza, where she treated children with gunshot wounds to the head
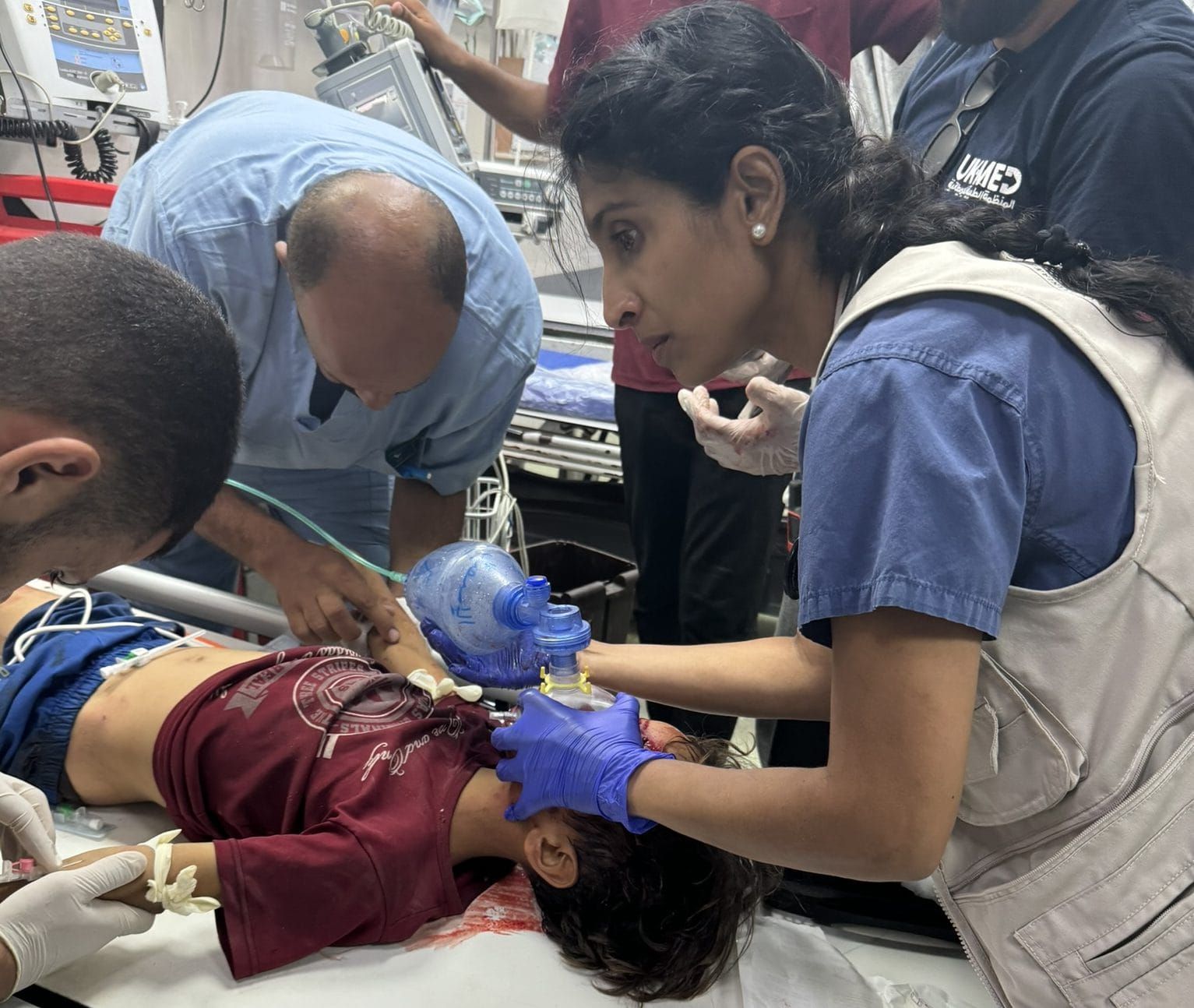
Dr. Mimi Syed embarked on her first four-week mission to Gaza in August 2024 with the Palestinian American Medical Association (PAMA) at Nasser Medical Complex in Khan Younis. Dedicated to serving Gaza’s devastated healthcare system, she returned nearly four months later in December 2024 with MedGlobal to Shuhada Al Aqsa Hospital in Deir al-Balah. Throughout her two months in Gaza, Syed became well acquainted with Israel’s ecology of war, witnessing the swift destruction of health care across the Strip.
Syed is a U.S. board-certified emergency medicine physician, born, raised, and trained in Chicago, Illinois. She is currently an assistant clinical professor at the University of Washington and Washington State University. Her missions in Gaza were the first of her career. On Aug. 20, with a suitcase full of baby formula and medical supplies to treat malnourished children, Syed was refused entry to Gaza for her third mission.
Syed spoke with Prism about Israel’s man-made apocalypse in Gaza, Israel’s targeting of women and children, the long-term effects of genocide, the rapid devastation of Gaza’s landscape, and the sustained impact of Israel’s blockade.
This interview was conducted during a fragile ceasefire in February. Although violence against Palestinians never halted during the ceasefire, Israel resumed the genocide in full force on the eve of March 18. Gaza’s healthcare infrastructure has been completely obliterated since. According to the World Health Organization, the remaining 18 of 36 hospitals in Gaza have reached their breaking point.
This interview has been edited for clarity and brevity.
Marah Abdel Jaber: What was your impression of Gaza during your first mission in August [2024]?
Mimi Syed: I watched the genocide livestreamed on my iPhone, but I was completely shocked by the destruction. Every single building was collapsed, there was rubble everywhere, and small children were walking around completely unattended. The most terrifying thing to me was the constant sound and proximity of munitions all around. The hospital was another level of annihilation that I never thought I would witness in my life. It was overcrowded; the temperatures were so high in August, and there was no air conditioner. And again, children without any adult supervision were walking around the hospital in groups. I was surprised by how close the munition was to the hospital, which was considered a humanitarian zone. And all of the patients were coming from “humanitarian zones” almost every time.
Abdel Jaber: What were the conditions in Nasser Medical Complex and Shuhada Al Aqsa Hospital when you arrived?
Syed: Al Aqsa Hospital was bombed shortly before I arrived. It was different because, in addition to having encampments on the grounds of the hospital, displaced people were also living inside. We didn’t see much of that at Nasser. Unless they were family of the patients receiving care, they weren’t allowed to live in the hospital. It seemed to me that the situation at Al Asqa was much worse. Of course, I’m comparing August and December. There was sewage everywhere, and the population that we were seeing was almost all children, coming in with all sorts of injuries. The illnesses were also distinct. I noticed that the patients coming in were more of a disaster of an illness than an injury, and [the aftermath of injury], like infection, poor healing, dehydration, and malnourishment. I also wasn’t working as much in the trauma bay as I did on my first mission. I was solely in the trauma bay at Nasser, but I was able to see some of the non-trauma cases. At Al Aqsa, I worked in the pediatric emergency department more. It was significantly worse than I imagined.
I remember pools of blood being moved back and forth by the janitor because they don’t have cleaning supplies. They would be putting dirty water on the floor after mass casualty incidents, and it was like a sea of blood being moved back and forth …
Dr. Mimi Syed
Abdel Jaber: How did you alter your practice to accommodate the conditions in Gaza?
Syed: I smuggled something called a laryngoscope. It’s a life-saving tool—we use it to maintain the airway if someone can’t breathe or is getting close to dying. It’s about the size of my palm for an adult, and for a child, it’s even smaller. They didn’t have any laryngoscopes in Gaza, or if they did, the batteries were dying, so we couldn’t use them. I was able to get them donated from my hospital, so I smuggled two in: one adult, one child. I reused them about 50 times, although these are meant to be thrown away after the first use. Similarly, in the U.S., you only use one pair of gloves per patient, but both times I used the same pair of gloves for every patient in a single mass casualty incident, because there were no gloves. There was no soap during either mission, and at times, there was no running water. I brought my own hand sanitizer, but I ran out. We would have blood on our hands and our clothes; everything was covered in blood. I noticed that the tubing of the ventilator had flies and black mold inside because it was being reused over and over again. The tubing for a vent has to be changed with every single patient, but it hadn’t been changed the entire year because there is no alternate available. Ambu bags, which are used to breathe externally for someone who is intubated, were also filled with black mold. They were reused, although they need to be thrown away after every patient. There were no mattresses on the cots. Civilians who came in with open injuries, bleeding, had to go on a hard metal cot, and there were only four of those, so we primarily treated patients on the ground. Even for life-saving procedures. There was nothing to clean the floors with. I remember pools of blood being moved back and forth by the janitor because they don’t have cleaning supplies. They would be putting dirty water on the floor after mass casualty incidents, and it was like a sea of blood being moved back and forth, because they were preparing for the next casualties. We had two types of sedatives: Propofol and Ketamine. These medications are inactive at a certain temperature. We would be giving horse-size doses to people, like little children, but because of the heat in August, they were ineffective. Essentially, people were going without any pain meds or analgesia because there was just nothing to give. Antibiotics were scarce. We were using one type of antibiotic for everything, and patients were coming back with likely drug-resistant, recurrent infections. I saw a culture and sensitivity report on an infected wound, and all of the drugs were resistant except one, which we didn’t have. That’s unheard of. This was the case for most people in Gaza.
Abdel Jaber: What preparation did you have for your missions?
Syed: On my first mission, I brought the two laryngoscopes, a box of gloves, and some antibiotics under my name to show Israel’s Coordinator of Government Activities in the Territories they were for me, but I was planning to use them for patients. The second time, I took similar items, but I only had one laryngoscope. I was also able to take a pediatric vent and HEPA filters. Before I went, one of the directors said that they were seeing a very high number of infections in neonates because there were no HEPA filters attached to the vents. Babies were dying from dirty vents pushing bacteria into their lungs. I tried to take a handheld ultrasound machine, but it was not allowed.
Abdel Jaber: What kind of injuries did you treat? What might they indicate about the weapons being used?
Syed: Both times, we saw small children under 12 years old with gunshot wounds. I saw many more children with gunshot wounds at Nasser because I worked primarily in trauma. I saw children with single shots to the head, chest, and abdomen every day for four weeks. I documented around 18 cases in voice notes, videos, pictures, or CT scans of children who were shot. My common practice was to ask whoever brought them in what happened. They would usually say the child was shot by a drone sniper.
Abdel Jaber: Did any stories stick with you?
Syed: One such case was a four-year-old girl named Mira. She was eating breakfast in her tent on Aug. 24, 2024, and a quadcopter shot her in the head. Many other casualties came in at the same time, including other children with gunshots to the head, and an airstrike in the so-called humanitarian zone—Mawasi at the time. Similar to Alaa, the girl I spoke about with NPR, kids and adults with neurotrauma or penetrating wounds to the head are usually left as unsalvageable during a mass casualty incident. Mira was marked unsalvageable, but she was still moving, so I intubated her with the laryngoscope I smuggled, and I was able to save her life. We brought a neurotrauma surgeon with us, so I ran up four flights of stairs, grabbed his arm, and said, “Come with me. We have to go take a look at this girl.” He took her into the OR [operating room] and saved her. She is alive and well today, but still needs medical evacuation. She’s one of thousands of children in this condition. Since my return to the U.S., her mother sustained a traumatic amputation to her leg due to another airstrike, and now needs medical evacuation. Over 70%, close to 80%, of the patients I saw were women and children under the age of 12.
Abdel Jaber: What kind of injuries did women and children often have?
Syed: We saw many traumatic shrapnel injuries, specifically neurotrauma with brain matter out. That was the case of Alaa. She has nothing but skin covering a big part of her brain. If she falls on rubble, because there are no roads anymore, she can suffer severe brain damage and die. She needs a bone graft and a titanium plate, neither of which can be offered in Gaza. We saw a lot of recurrent infections in addition to trauma on my second mission. Because there’s no sanitation and sewage everywhere, I remember many cases of small children with chronic diarrhea from water contamination. The Israeli military blocked the entry of supplies to purify water—the chlorine membranes, which clear out salt. There’s a very high salt content in the water, so we were also seeing extremely high numbers of kidney failure in small children, which is not common. This is from two major things: the first, a skin infection caused by streptococcus from poor sanitation. It is extremely preventable, but if untreated, it leads to kidney failure. Those are the most preventable types of infections/aftermath of infection that you don’t see in the United States because of a simple antibiotic that we have in this country, which you cannot get in Gaza. Second is the high salt content. Kids are getting kidney failure because of the high salt content in water. E. Coli poisoning is so high that kids would get chronic diarrhea, causing them to die of hemorrhagic GI [gastrointestinal] bleeding. Completely preventable. You won’t see that in the U.S. It just doesn’t happen.
Abdel Jaber: What are the long-term implications of these injuries?
Syed: So if a child happens to survive, they probably have a long-term disability, because many of the children in Gaza have been malnourished and are now suffering from chronic illness. That is the time to develop, and when you’re lacking significant, essential nutrients, it causes lifelong illnesses. A very good example is the birth rate, children, and decreasing population size. There is a 300% rise in miscarriages after Oct. 7 for pregnant women in Gaza. That is an unheard-of, unfathomable number. When children are born, mothers are so significantly malnourished that they’re having children with conditions like spina bifida. You can prevent spina bifida with folic acid, but mothers don’t have that in Gaza. They don’t have basic nutrients. It’s put in our bread here in the United States. It’s so easy to get that you rarely see it here. But that child will have a debilitating chronic illness. This is not just going to go away with a ceasefire. Wounds are not healing because there is no protein in the market. Wounds would just stay open or get infected. We talked about children like Mira and Alaa, who have neurotrauma. You can’t have a normal life if you’ve had a bullet in your head at some point. You will continually need medical care. You are forever disabled. The largest amputee population in pediatric patients is in Gaza. And not just a single amputation, but double, triple amputees. That’s a maimed population.
Abdel Jaber: What was your experience of entering and exiting an active genocide?
Syed: What I felt, and continue to feel, is guilt—guilt that I get to leave while this continues to happen. When I left, and now when I mentor, all I feel is that humanity has abandoned Gaza. When you see small children of one, two years old supervised by a seven-year-old, it indicates that there is no humanity left. In December, I saw children walking alone in cold weather, no shoes, no warm clothing, no adults in sight, alongside an annihilated road. Almost every kid I saw was carrying an empty canister of water, hoping to find water, fill it up, and take it back to wherever they’re living. As a foreign aid worker entering and getting the privilege to leave, after I’ve shared my life and daily trauma with the people of Gaza, I feel nothing but guilt and anger. It doesn’t go away. I wake up with it every day. I sleep with it. Because the atrocities in Gaza don’t end. The ceasefire promised temporary shelter, heavy machinery to clean up the rubble, to fix the roads and the electricity grids that have been destroyed, and the water system that has been annihilated. None of those things has happened. Dr. Al-Farra told me, “You know, I need this type of medication for this little girl who has Guillain-Barré syndrome,” which is completely preventable. “If we had the medication, she would live.” The Israeli military blocked the medication that she needs. They used to allow it, but now they are not. What’s the reason for that? Other than cruelty, what’s the reason?
Abdel Jaber: What were conversations like among your peers regarding the fragility of life in Gaza?
Syed: I made lifelong relationships in Gaza. Many of the journalists are my very good friends, and I continue to speak to them. Ayman [Al Jadi], a friend from social media, was killed while I was there. I still get emotional about it. I was supposed to see him the day after he was killed. He was going to interview me, but he came on Friday and said, “I’m so sorry I wasn’t able to come sooner, my wife is in labor, and I’m going to go meet her at the hospital.” I said, “Oh my God, what are you doing here? You should be at the hospital with your wife! Congratulations!” This was his first child. I said, “Don’t worry about it. We will catch up, I’m here for a while.” And he left. I have a video of him from that day because a journalist recorded us. I didn’t know until after the fact. I was still messaging him, saying, “Congratulations, I hope everything’s going okay.” And he said, “No, everything’s fine, I’m so happy! I will see you tomorrow at noon.” Then, I woke up the next morning, and my phone was filled with messages saying “Ayman is dead. Ayman is killed.” The car he was in, which was clearly marked “press car,” with four other journalists, was struck right in front of the hospital where his wife was about to give birth. I didn’t believe it at first. I thought, “That’s impossible, I just saw him, it’s got to be a mistake.” But when I spoke to the other journalists, it was real. His wife had the baby the next day, and she was supposed to name him Abdul. People encouraged her to name him Ayman, and she said, “No, it’s Abdul. Why would I name him Ayman?” So they told her the news, and she named her son Ayman. It was a reminder of how fragile life is in Gaza. There is no permanent fixture in Gaza. No relationship you make is protected there. The same thing happened with Khaled Nabhan [a grandfather whose grief was witnessed across the world]. Two days after we met, he was killed in an airstrike.

Abdel Jaber: As a foreign aid worker, did you have any sense of security in Gaza?
Syed: Among foreign physicians, no one felt safe in Gaza. There was a small sense of security, but we all knew it wasn’t true. Everyone is fair game to be killed. In August, I was standing on the roof of the hospital seeking reception to call my husband while a drone sniper was shooting down. One of the surgeons came, grabbed me, and took me down. No one was safe. When I was at Nasser, there was a car bomb on the hospital grounds while we were in the ER. The shock waves went through my eardrum. This continued to happen. We were always trying to be positive, but we all knew that there was no security. When we spoke to the people of Gaza, I would always ask the same question: How could you be so patient and kind? I am angry every day. I have resentment. They would reply: “We can’t be angry at something we don’t have control over. We are responsible for ourselves, and one day this will end, and we’ll still have to be responsible for our actions.” I don’t have that much patience, but they are people with such strength and resilience and kindness. I never witnessed that level of camaraderie in my life. We wore American flags on our vests because of our NGOs [nongovernmental organizations], and I thought people would be so angry with me, but it was the opposite. People would come up to me and say, “We thank you for being here and standing in solidarity with us when you have left your safety and your own family. It gives us hope.”
Abdel Jaber: How are your conversations about Gaza in the U.S.?
Syed: They’re very unfortunate. People live in a bubble, and they bury their heads in the sand. Almost all of us who have gone on missions asked our respective professional colleges to make a statement about Gaza and the targeting of healthcare workers, and we have been told, “No, this is a political thing that we don’t want to get involved in.” But they have made statements about Ukraine. It is hypocritical and very cowardly. As humanitarians, as healthcare workers, it’s our job to speak up when witnessing human rights being violated and healthcare workers being deliberately targeted. I met countless healthcare workers who were imprisoned and tortured just because they were in the hospital on Oct. 7, 2023. They had no charge against them. Some were imprisoned and tortured for months at a time, and others were killed. There’s a case of an orthopedic nurse who was blinded, amputated, and debilitated, because he refused to leave his patient in the OR. Israeli soldiers shot and maimed him. And what did he do? He returned to the hospital immediately after his release. In the U.S., many people think it’s not affecting us directly. We are directly funding this with our tax dollars.
Abdel Jaber: What did Gaza teach you?
Syed: To continue to fight. I will never stop speaking up for Gaza. Until my last breath, I will advocate for their existence, because they have that right.
Editorial Team:
Tina Vasquez, Lead Editor
Carolyn Copeland, Top Editor
Stephanie Harris, Copy Editor
Author

Marah Abdel Jaber is a Palestinian writer, researcher, and creative. She was the team lead on Palestine Square’s “Firsthand Accounts from U.S. Medical Missions in Gaza” series, collecting testimonies
Sign up for Prism newsletters.
Stay up to date with curated collection of our top stories.