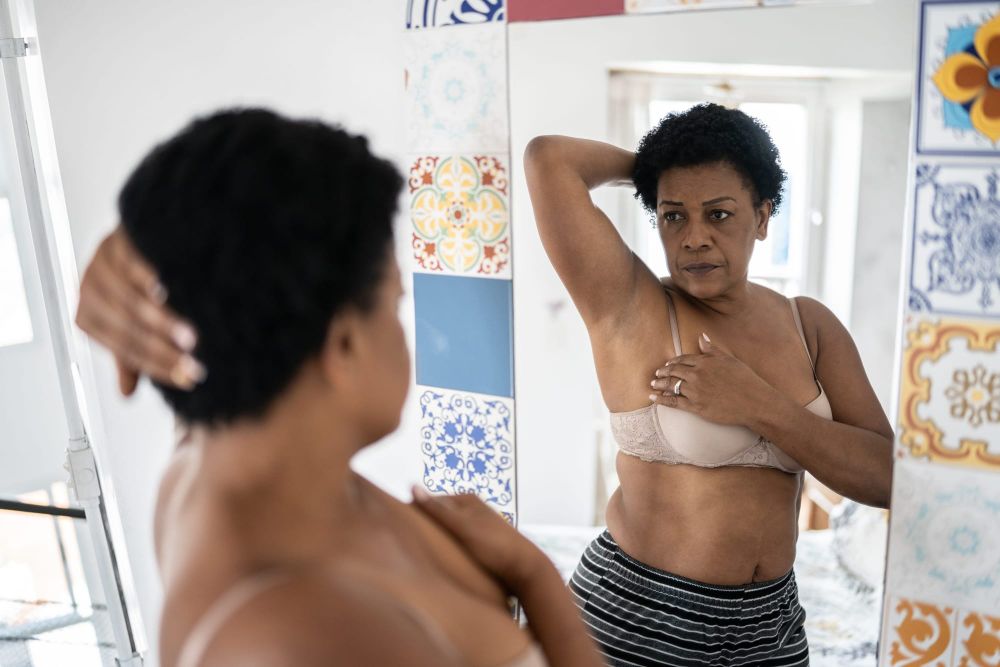Patients react to Trump’s closure of the long-COVID office: ‘I am horrified to think about care becoming less accessible’
Millions of people in the U.S. with long COVID are facing further government abandonment rather than receiving necessary care
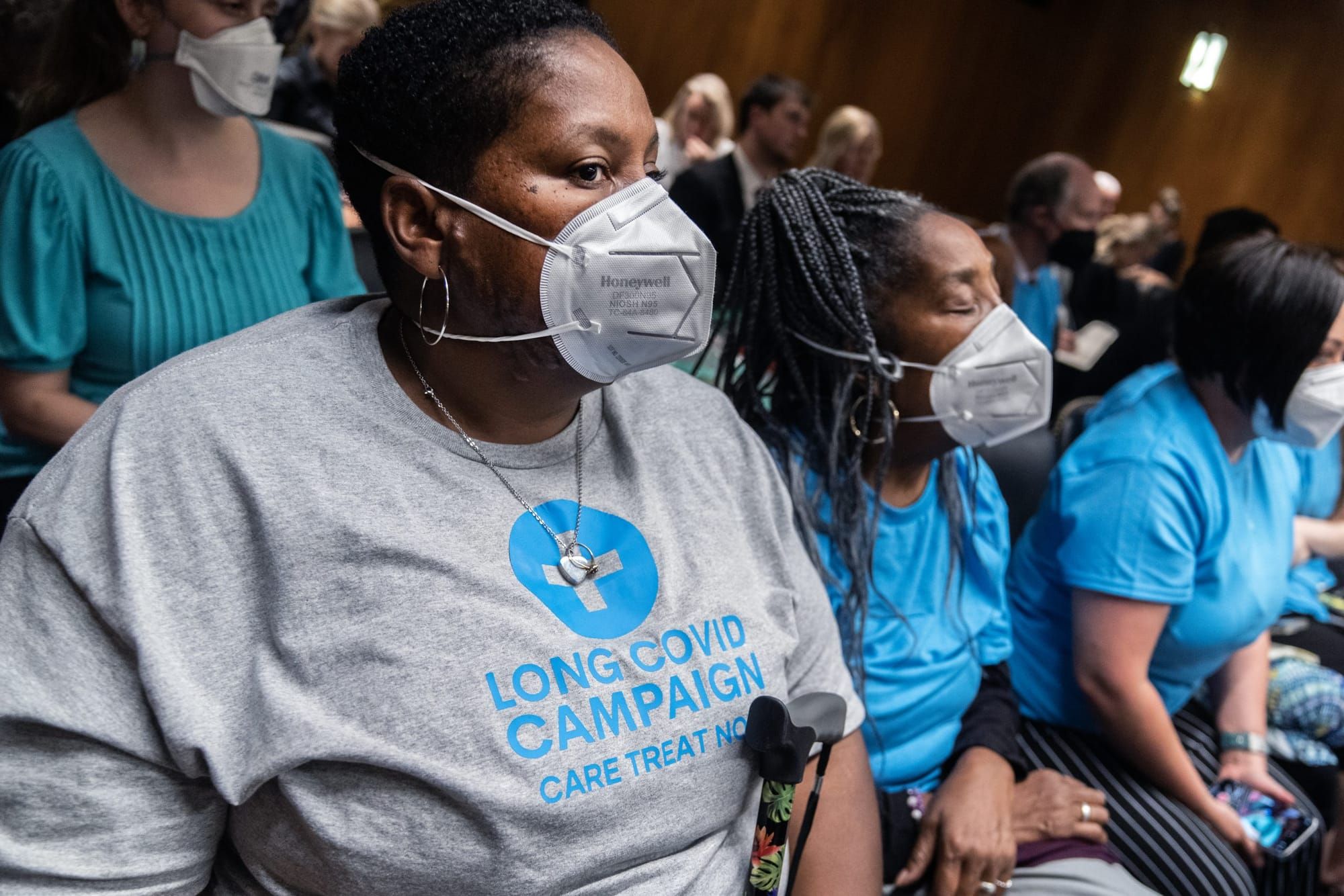
The government response to COVID-19 under the Biden and Trump administrations has been lackluster, particularly for those dealing with long COVID, a disabling condition with a myriad of symptoms. According to a study released in May, conducted by researchers at the Icahn School of Medicine at Mount Sinai, long COVID can cause long-term changes in the heart and lungs. Even mild or asymptomatic COVID-19 infections can have serious cardiovascular consequences, according to the study’s findings. But the risks are not limited to the cardiovascular system alone.
An estimated 23 million people in the U.S. have long COVID, but their care and treatment needs have long been neglected, and under President Donald Trump, the situation is even more dire.
The Trump administration’s reorganization of the Department of Health and Human Services (HHS) led to the closure of the Office of Long COVID Research and Practice (OLC). After the National Institutes of Health (NIH) rescinded threats to revoke research grant funding in March, the NIH’s $1 billion Researching COVID to Enhance Recovery (RECOVER) Initiative now appears to be safe from cuts. But in March, former OLC employees, along with some current employees at the time, told Politico that “closing the office will hurt collaboration and communication among researchers as well as social services for patients.”
To better understand the realities facing people living with long COVID, Prism spoke with four patients about their current access to care and the anticipated effects of further government abandonment.
Responses have been edited for length and clarity.
Lida Richardson, 30, student and writer living in New York
I think I’ve had long COVID for about a year and a half, but I only came to fully realize it in the past few months. I had my second COVID infection in September 2023, which led to fatigue and worsening chronic symptoms. I was working at a restaurant at the time and also taking classes online, and I suddenly had a lot of trouble keeping up. I’ve had chronic migraines since I was 25, and I’ve always had some level of fatigue, so I had trouble identifying how much worse things actually were.
For a while, I just kind of pushed through the fatigue. I took really long walks, was really busy with a lot of activism, and was working pretty hard to keep up with school. And it was a classic post-exertional malaise (PEM) situation. The fatigue and other symptoms started getting progressively worse, and by the time I got to December 2023, I was just completely burnt out.
Until I started at the New School, my insurance had still been at home in Boston, so I couldn’t go to a primary care physician in New York. But once I enrolled in the New School, I got student insurance, and I finally went to a PCP in January. I really lucked out with him—he pretty much immediately identified that what I had was probably myalgic encephalomyelitis/chronic fatigue syndrome, but wanted to rule other things out, and helped me understand what PEM was.
Over the past months, my symptoms have pretty dramatically worsened. I managed to do a consultation at NYU Langone’s Post-COVID Care Program last month; I lucked out and got an earlier appointment because of a cancellation. The nurse practitioner there was really validating and helpful. She prescribed a number of supplements and also referred me to some specialists, all of whom have long wait times, which is a big barrier to care. That has meant a lot of sitting around and hoping I don’t get worse, and trying to stay on top of everything nonnegotiable.
Overall, I’ve been really lucky. I had to get past a lot of my “just work through it” programming, but I have good insurance from school, and I’m enormously privileged not to be working right now. I’m really concerned for the people who are in the position I was in last year, trying to muscle their way through and running into a wall, but unable to take a break from work or see doctors who will do anything but gaslight them. I also worry a lot about people with mental health comorbidities like me. I’m white and a student and have been in treatment for a long time, which I think has helped me be taken seriously. I can only imagine how many people with mental illness have been completely invalidated about long-COVID symptoms.
This was all before the closure of the HHS (long COVID) office. I am horrified to think about care becoming less and less accessible and, like with all of these systemic failures, the most vulnerable people being harmed first. In my experience, it took enormous time and effort to even realize I had long COVID, and less support means fewer people will know they have it and will be told to do the opposite of what’s healthy for them: Exercise more or work harder. I think it’s an enormously important time for long-COVID journalism, peer-to-peer support, and disability solidarity. I don’t know if I ever would have figured out what was going on with me if I didn’t have disabled friends to give me advice and validate my experience.
Leslie Lee III, writer, English teacher, and host of the podcast “Struggle Session” living in Virginia
Seeking medical treatment has largely been a waste of time at best, and actively harmful to my condition at worst. Most doctors and caregivers are tragically ignorant about COVID and long COVID. They don’t take precautions—even when they’re treating patients who are seeing them because they have been disabled by a COVID infection. You’re constantly asked to take tests that everyone knows will not really show anything because the tests have not been adjusted to track long COVID, and medical knowledge of post-viral conditions in general was already in a terrible state. The entire medical industry should be playing catch-up, but they’re not. They’re being dragged along by the reality of patients coming with these health problems after COVID infections.
When I was able to see someone at a long-COVID clinic, it was nice to work with medical staff who were informed about long COVID, even if some of that information was inaccurate. My caregiver was very helpful in providing me a pacing guide, and that was perhaps the most helpful treatment from any provider so far: a one-page guide to earnestly resting. However, they also recommended gradual exercise therapy, which for many people with long COVID is both ineffective and actively harmful. Even the staff at the clinic knew full well the limitations of everything they had to offer. Most of the things that have helped me have come from listening to other patients in the long-COVID community.
The type of research and the amount of research done under the Biden administration was often wrong-headed and inadequate, and people in the long-COVID community were immensely frustrated already. Closing the long-COVID office is making a bad situation worse, but it’s going to get to a point where the world just can’t ignore the problem anymore. Too many people will be too sick to keep pretending that governments don’t have to take action.
Everyone, regardless of health or age, is vulnerable to COVID. COVID infections are linked to heart attacks, strokes, blood clots, aneurysms, cancer, diabetes, hair loss, tinnitus, erectile dysfunction, and more. Masks work—use them.
Ultimately, I wish people’s intersectional justice and community care practices weren’t just limited to people who aren’t disabled.
Ren Kaltenheuser
Ren Kaltenheuser, 30, lead researcher and graduate student living in New York
My experience has been profoundly shaped not just by the symptoms, but the holistic overview of the costs of having long COVID. In relation to accessibility post-developing long COVID, there has been a tangible cost of spaces not feeling accessible or safe, and the radiating effect of that on personal relationships and my overall mental health.
The cost of having long COVID has also been a lot of emergency room visits, time spent commuting, time spent missing life, and time spent waiting in medical offices that often don’t have answers. The cost burden has been more than financial—it’s also been time and life and relationships.
In terms of trying to access care, I have spent months on waitlists, only to find out that they no longer take my insurance. I am currently on another waitlist for a long-COVID provider that I’ve waited over a year to see; I’ll meet them one month from now. Just the process of trying to get in is exhausting because there are so many hoops and so few providers. This becomes more difficult considering how few providers are trained and the fact that it often takes a multidisciplinary approach, depending on your symptomatology.
The closure of the long-COVID office will make it harder than it already is to access care. It could impact the validity of the diagnosis and how it’s interpreted by the medical community. There are a multitude of ways it could impact individuals living with long COVID, especially those who haven’t been able to get a diagnosis yet or those who are seeking disability leave due to the effects of long COVID on their lives.
Ultimately, I wish people’s intersectional justice and community care practices weren’t just limited to people who aren’t disabled. Wear a mask.
Heena Sharma, 36, educator, facilitator, and program manager living in Harlem
It took me some time to even conceive of my “symptoms” because of the ways my experiences of trauma and violence left me disconnected from my body. My dissociation and self-gaslighting could have kept me in the dark for a long time, but it was only through working through trauma and complex post-traumatic stress disorder and re-remembering my body that I was able to start recognizing my symptoms. I share this to say that the gaslighting and minimizing I did to myself were mirrored by what I experienced by doctors.
Even though I was able to get services from a long-COVID clinic, it was a mixed experience. The clinic was located on the pulmonary hospital floor, where no one was masked, including elderly folks using different mobility aids. My doctor wore a mask, but the nurse taking my vitals did not, and barely reacted when I explicitly said I was there for long COVID. Most of the doctors in the clinic who would have been best suited to work with me did not take insurance, and a cardiologist I waited three months to see called me the day before and said they don’t see patients with postural orthostatic tachycardia syndrome (POTS), which I was ultimately diagnosed with.
I was prescribed physical therapy, but I was routinely and sharply judged and berated by my physical trainer for just not working hard enough. Because I “didn’t look” sick, any feedback was received as lazy complaining. Despite seeing my heart vitals, my physical trainer would say I just needed to push myself harder. She was a cis[gender] white woman who I felt was reprimanding me as though I were a delinquent student. Although I made some gains and self-discovery through PT, it was only because I resolved to take what I could get through my state-sponsored insurance.
This clinic at a world-renowned hospital in New York offered crumbs that I was lucky enough to taste, and yet even those crumbs were deemed too generous by this government and HHS, considering the shutdown of the long-COVID office.
Editorial Team:
Tina Vasquez, Lead Editor
Carolyn Copeland, Top Editor
Stephanie Harris, Copy Editor
Author

Reina Sultan is a Lebanese Muslim movement journalist and one of the co-creators of 8 to Abolition. You may have seen her work in Vogue, VICE, ELLE, Business Insider, SELF, Prism, Yes! Magazine, and m
Sign up for Prism newsletters.
Stay up to date with curated collection of our top stories.