Oregon’s expansion of Medicaid coverage to incarcerated people sparks hope and skepticism
The new program aims to improve reentry outcomes, but critics question its effectiveness amid systemic health care issues in correctional facilities
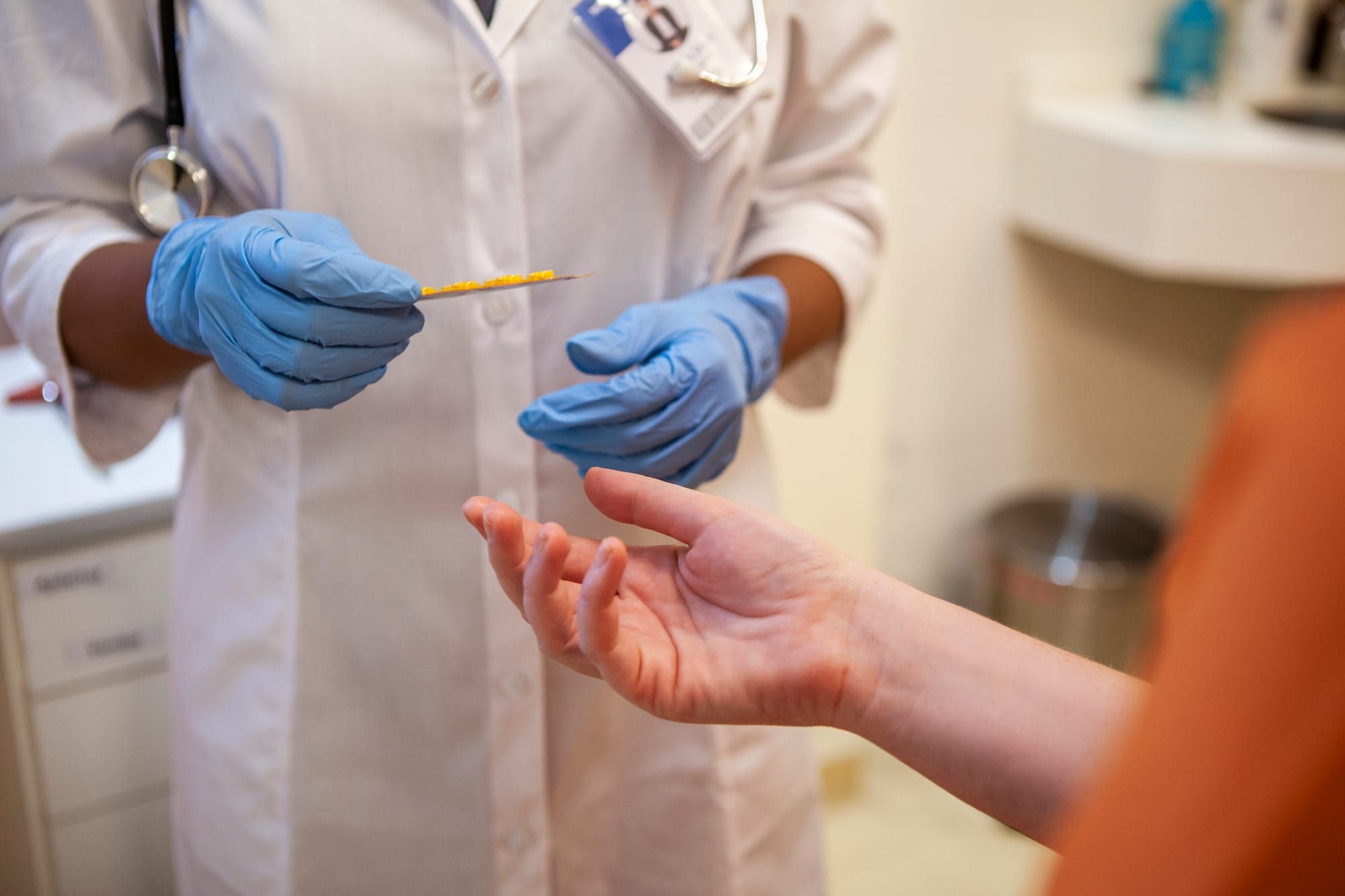
In July 2024, federal officials approved Oregon’s request to provide Medicaid services to eligible incarcerated people 90 days before their release. Set to launch in January 2026, the Oregon Health Authority said the program hopes to support an individual’s reentry into society and, ultimately, reduce recidivism rates. Those who qualify will also gain access to lab and radiology services, mental health assessments, and medications needed to treat opioid addiction. To receive this federal funding, institutions must follow the Federally Consolidated Appropriations Act (FCAA) and voluntarily opt-in to the program.
“This funding will be a huge tool for jail and prisons in helping those incarcerated receive proper discharge planning for successful reentry into the community, ensuring the continuation of care for one of our most vulnerable populations,” said Capt. Lee Eby, Clackamas County jail commander, in a July 3 statement.
While this program is seen as a win for progressive, solutions-based public safety and public health policies, some remain skeptical of its implementation. Providing health care to incarcerated people is costly, historically ineffective, and inadequate. While tapping into federal tax dollars may relieve some of the burden, it doesn’t change the abysmal record that jails and prisons have at providing these health care services in the first place.
Legislation surrounding incarcerated health care reached a turning point in 1976 when the Supreme Court ruled in Estelle v. Gamble that failing to provide a minimum standard of health care for incarcerated people was a direct violation of the Eighth Amendment’s prohibition against “cruel and unusual punishment.” This case came at a crucial time in U.S. carceral history: 1970 is often identified as the beginning of the country’s “era of mass incarceration,” when issues like crime-centered campaign rhetoric and stricter sentencing laws led to the deliberate growth of the nation’s prison population.
Since then, the U.S. incarcerated population has increased by 500%—a growth that has only exacerbated the cost and ineffectuality of providing health care to those behind bars. The No. 1 expense in Oregon’s Department of Corrections (DOC) general fund budget for 2023-2025 is health services, at just slightly over $418 million. Oregon also has one of the fastest-growing aging prison populations due to mandatory minimum sentences set in 1994 by Ballot Measure 11, which has only increased incarcerated health care costs to account for higher rates of chronic illnesses and other health complications among the elderly.
Expense, however, isn’t the only reason behind the failings of incarcerated health care. Facilities like jails and prisons are repeatedly shown to be ineffective community health service providers, occupied with increasingly draconian calls to further incarcerate and punish those with addiction and mental health disorders instead of rehabilitating them. In early 2024, Multnomah County Sheriff Nicole Morrisey O’Donnell commissioned a National Institute of Corrections assessment of her county jails, in response to an abnormally high rate of suicide among people incarcerated there. Independent auditor Margaret Severson found that, despite a corrections health budget of about $31.5 million in 2024, health care behind bars was plagued by “serious health care and operations issues,” such as lack of patient privacy, inexact protocols, and understaffing.
“Time is of the essence,” Severson wrote in her assessment. “There are practices and omissions occurring in [these] jails that do not comport with constitutional standards, accreditation standards, and professional practice standards.”
Severson noted that she was neither provided with the requested information on how many incarcerated people received daily medications nor the number of medications administered on a daily basis, suggesting a lack of oversight on basic day-to-day operations and an overall lack of accountability and professional standards. Mental health and addiction services showed similar, if not worse, conditions. According to the report, no one was able to provide an estimate of the percentage of incarcerated people with mental illness and co-occurring disorders at the time. Severson also found no formalized substance abuse programs active in the jail system, despite the reversal of Ballot Measure 110 last September ending drug decriminalization efforts in Oregon. If drug possession of any amount is again a jailable offense, shouldn’t jails be equipped with the resources to address drug addiction?
The perils of incarcerated health care also affect prison staff. In April 2024, union nurses working in Multnomah County detention facilities called on the county sheriff to fire two supervisors for absenteeism and negligence; other grievances included forced overtime and not having enough staff to run basic medication lines at the juvenile detention center. Severson noted similar instances of forced overtime and nurse vacancies in her assessment, stating that the jail system suffered from being understaffed and deploying available staff “in ways that do not maximize their time and skills.”
Given this data, it should be no surprise that critics remain skeptical of Oregon’s approval to offer Medicaid to incarcerated communities, as it simply throws more money at a problem that cannot be corrected at its root through increased expenditure alone. Instead, a greater release valve is necessary. Kyle Hedquist, a policy associate at the Oregon Justice Resource Center who advocates for the clarification and expansion of medical and geriatric parole in the state, told Prism that this release valve must come in the form of a full repeal of Ballot Measure 11 and mandatory minimum sentencing. He said that the measure traps people in prison without the possibility of early medical release, even when they’re stuck in a “long, slow death” from health complications and diseases.
In a system concerned more with confinement than care, increasingly graying prison populations will only continue to drive up the cost and difficulty of providing health care to incarcerated people as a whole.
“Pie in the sky would be a whole repeal of Measure 11 to free up the parole board and prison system to look at these cases more freely,” Hedquist said. “Relieving that pressure valve will allow DOC to [better] use medical resources for the rest of the population.”
Editorial Team:
Rikki Li, Lead Editor
Carolyn Copeland, Top Editor
Rashmee Kumar, Copy Editor
The Right to Write (R2W) project is an editorial initiative where Prism works with incarcerated writers to share their reporting and perspectives across our verticals and coverage areas. Learn more about R2W and how to pitch here.
Author
Wesley Vaughan is a formerly incarcerated writer whose nonfiction has appeared in The Appeal, Inquest, Next City, Truthout, and with Vera Institute of Justice. He is a member of the Transforming Justi
Sign up for Prism newsletters.
Stay up to date with curated collection of our top stories.



